Can Acupuncture Help Fibromyalgia?
What a New Review Means for Patients

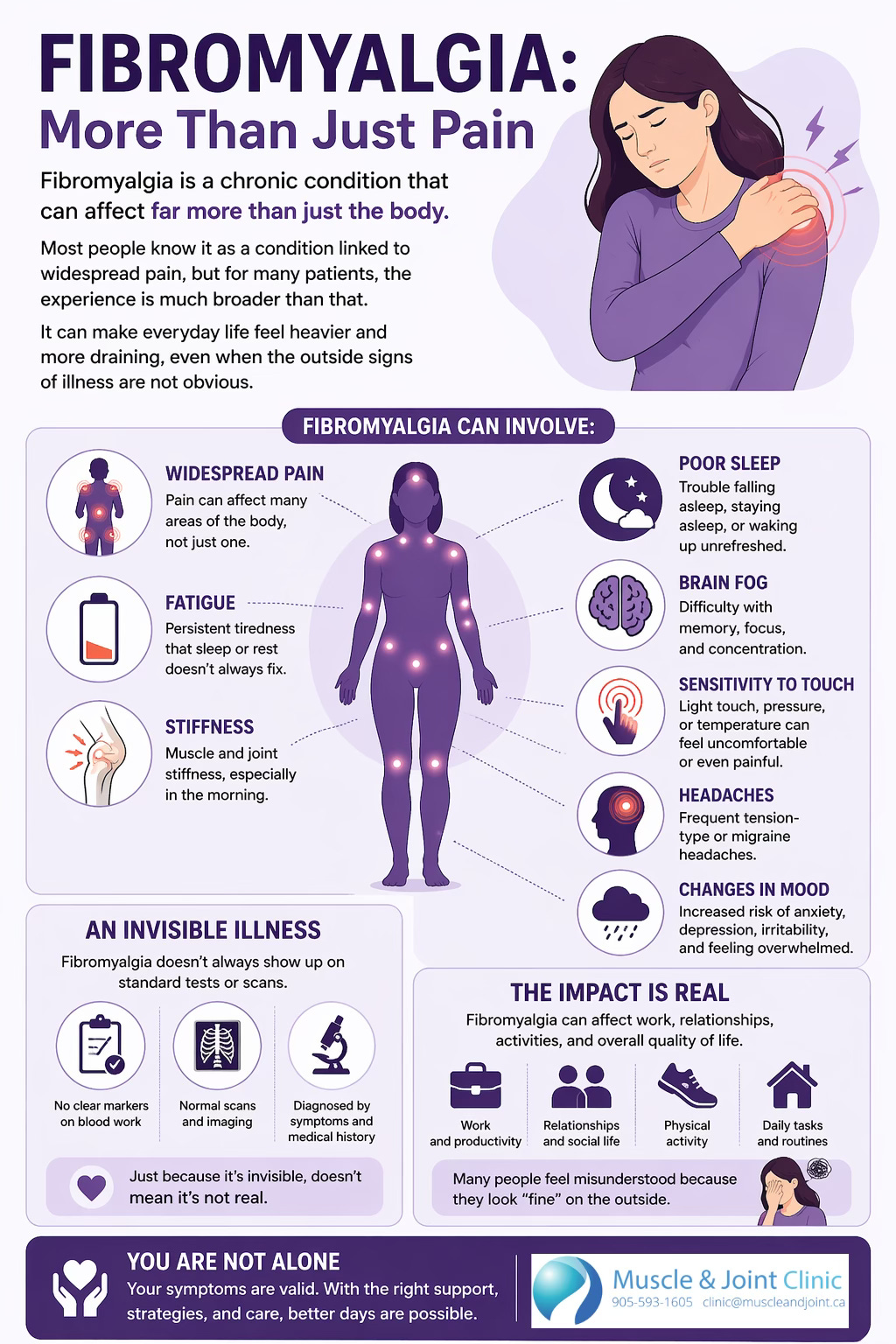
Fibromyalgia is a chronic condition that can affect far more than just the body. Most people know it as a condition linked to widespread pain, but for many patients, the experience is much broader than that. Fibromyalgia can also involve fatigue, stiffness, poor sleep, brain fog, sensitivity to touch, headaches, and changes in mood. It can make everyday life feel heavier and more draining, even when the outside signs of illness are not obvious. That is one of the reasons fibromyalgia can be so frustrating. Many people are dealing with real and ongoing symptoms, yet they often feel misunderstood because the condition does not always show up clearly on standard tests or scans.
At its core, fibromyalgia is thought to involve changes in how the nervous system processes pain. In many patients, the body becomes more sensitive to sensory input, meaning signals that should feel mild or manageable can start to feel much more intense. This is often described as central sensitization. In simple terms, the nervous system becomes more reactive, and the “volume” on pain processing gets turned up. That does not mean the pain is imagined. It means the nervous system is amplifying the experience of pain in a way that can make normal daily life much harder. This is part of why fibromyalgia can cause pain in multiple areas of the body, even without a single injury explaining it all (Jin et al., 2026).
Fibromyalgia also tends to create a cycle. Pain can disrupt sleep. Poor sleep can increase fatigue and make the body feel more sensitive. Fatigue can make it harder to exercise or stay active. Lower activity levels can contribute to more stiffness and poorer physical function. Over time, that combination can also affect mood, confidence, work ability, and overall quality of life. For many patients, fibromyalgia is not just about hurting. It is about feeling worn down, limited, and unsure of how to break out of that pattern.
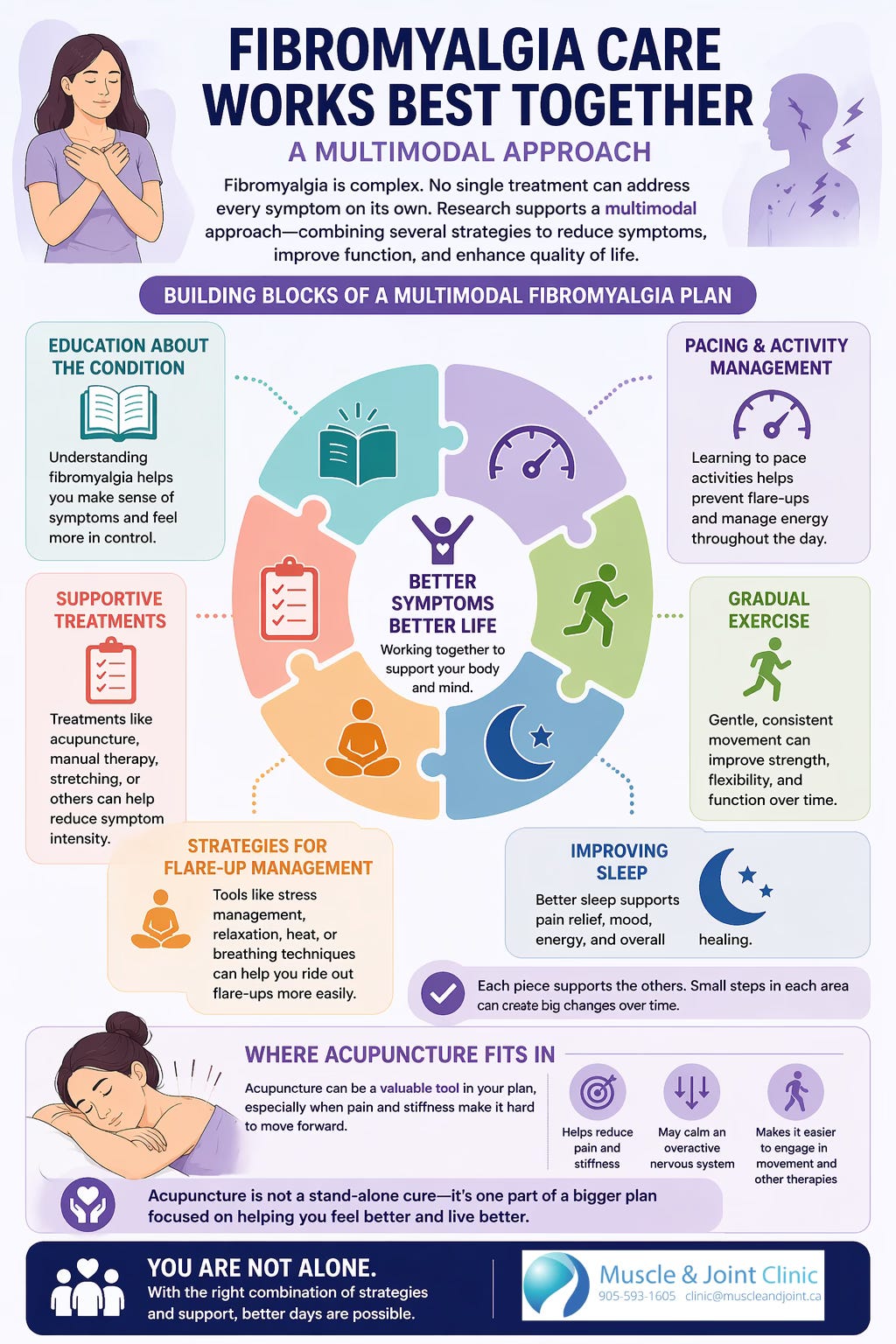
This is why treatment for fibromyalgia usually needs to be broader than simply trying to numb pain. Most current recommendations emphasize non-pharmacological care as the foundation of treatment. That often includes education, pacing, regular movement, exercise, and strategies to improve function over time. Medications may still play a role for some patients, but they are often used as part of a larger plan rather than as a complete solution. The challenge, of course, is that when someone already feels exhausted, stiff, and sore, even good things like exercise can be hard to start and even harder to maintain. That is where supportive therapies, including acupuncture, often enter the conversation (Macfarlane et al., 2017).
A recently published 2026 meta-analysis in the Journal of Pain Research looked closely at this question. The researchers reviewed 17 randomized controlled trials involving 773 patients with fibromyalgia to better understand whether acupuncture can help with the core symptoms of the condition. Their findings were encouraging in some important ways. The review found that acupuncture was associated with significant improvements in pain and stiffnessin the short term, and these benefits remained statistically significant in longer-term follow-up as well. The authors also found short-term benefits in areas such as quality of life, mental health, work ability, anxiety, depression, and energy. However, not every outcome improved in the same way. When the researchers pooled the data, they did not find clear overall improvements in physical function or fatigue across all studies, although some subgroup findings suggested that certain acupuncture approaches or treatment frequencies may influence those outcomes (Jin et al., 2026).
That distinction matters. It means acupuncture may be helpful, but it is not a cure-all. For patients, the most practical takeaway is that acupuncture may offer symptom relief in some of the areas that make fibromyalgia especially difficult to live with, especially widespread pain and stiffness. Even modest improvements in these symptoms can matter a great deal. When pain comes down and stiffness eases, even a little, people may find it easier to move, sleep better, tolerate exercise, or simply get through the day with less effort. That can create an opening for other parts of treatment to work more effectively.
The review also highlighted that how acupuncture is delivered may matter. The authors found that higher treatment frequency was linked with better short-term improvements in some outcomes such as physical function and stiffness. They also found that acupuncture combined with electrical stimulation showed potential additional benefits for fatigue and tender point reduction. This suggests that acupuncture is not a simple yes-or-no treatment. The details of the treatment plan, how often it is done, what type is used, how long treatment continues, and what it is paired with, may all influence results (Jin et al., 2026).
For many patients, one of the most reassuring parts of this research is that it supports the idea that fibromyalgia management should be multimodal. Fibromyalgia is complex, so treatment often works best when it addresses more than one layer of the condition. That may include education about the condition, help with pacing activity, exercise that starts at a manageable level, strategies to improve sleep and reduce flare-ups, and supportive treatments that help reduce symptom intensity. Acupuncture may fit into that picture as one useful tool, especially for people whose pain and stiffness are making it hard to move forward with other parts of rehab.
At The Muscle & Joint Clinic, we understand that fibromyalgia often leaves patients feeling like they have tried many things without getting the clarity or support they need. Our goal is not to oversimplify the condition or promise a quick fix. Instead, our focus is on helping patients create a plan that is practical, individualized, and grounded in what their body can tolerate right now. For some patients, acupuncture may be a helpful part of that process. It may help reduce pain, calm some of the body’s reactivity, and make other aspects of treatment feel more manageable. For others, the main focus may be on education, movement strategies, pacing, or building back confidence in activity.
What matters most is finding an approach that respects how real fibromyalgia symptoms are without encouraging fear or hopelessness. Patients with fibromyalgia often benefit from care that is gradual, consistent, and tailored to their individual presentation. That includes recognizing that flare-ups can happen, progress may not always be linear, and success is often measured in meaningful everyday changes: sleeping a bit better, having less morning stiffness, being able to walk longer, managing work more comfortably, or feeling less overwhelmed by symptoms.
One of the reasons acupuncture may appeal to patients with fibromyalgia is that it offers a non-drug option that can be integrated into a broader care plan. Some people are looking for alternatives because medications have only helped a little, or because side effects have made them hard to continue. Others want something that may help them feel more in control of their symptoms while they work on exercise, pacing, and lifestyle strategies. The newer evidence suggests that acupuncture may indeed have a role here, particularly for easing pain and stiffness, even if it is not the complete answer on its own (Jin et al., 2026).
It is also worth remembering that fibromyalgia symptoms are not just physical. The condition can affect mental and emotional well-being too. Chronic pain and poor sleep can wear people down over time, and when symptoms interfere with work, family, and social life, it is common to feel frustrated, anxious, or low. The meta-analysis found short-term improvements in depression, anxiety, and mental health measures with acupuncture, which may reflect the fact that reducing physical symptom burden can sometimes also improve how people feel overall. Again, that does not mean acupuncture replaces mental health support when needed, but it may be one piece of a more comprehensive support system (Jin et al., 2026).
For patients wondering whether acupuncture is “worth trying,” the answer is often less about whether it is a miracle treatment and more about whether it may help enough to support progress. Fibromyalgia rarely responds to one single intervention. But if a treatment can lower pain, reduce stiffness, and make movement or sleep a little easier, that can be valuable. The key is to place acupuncture in the right context: not as a standalone cure, but as one possible part of a larger strategy aimed at improving function, symptom control, and quality of life.
If you are living with fibromyalgia, it can be helpful to know that there is growing research looking at supportive options like acupuncture, and that your experience of pain and fatigue is real even when it is complex. Fibromyalgia can be difficult, but that does not mean you are out of options. The best treatment plans are often the ones that are thoughtful, flexible, and built around the person rather than just the diagnosis.
At The Muscle & Joint Clinic, we work with patients to help them better understand what may be driving their symptoms and what kinds of treatment strategies may fit best. For some, acupuncture may be one of those strategies. For others, the plan may focus more heavily on education, pacing, and progressive movement. In either case, the goal is the same: to help reduce the symptom burden, improve function, and support a steadier path forward.
Fibromyalgia is not “just pain.” It is a condition that can affect the whole person. And that is exactly why care needs to look at the whole person too.
References
Fitzcharles, M. A., Cohen, S. P., Clauw, D. J., Littlejohn, G., Usui, C., & Häuser, W. (2021). Nociplastic pain: Towards an understanding of prevalent pain conditions. The Lancet, 397(10289), 2098–2110. https://doi.org/10.1016/S0140-6736(21)00392-5
Jin, L., Zhou, Y., Li, L., Song, F., & Zhou, Y. (2026). Efficacy of acupuncture in patients with fibromyalgia syndrome: A meta-analysis. Journal of Pain Research, 19, 568235. https://doi.org/10.2147/JPR.S568235
Macfarlane, G. J., Kronisch, C., Dean, L. E., Atzeni, F., Häuser, W., Fluß, E., Choy, E., Kosek, E., Amris, K., Branco, J., Dincer, F., Leino-Arjas, P., Longley, K., McCarthy, G. M., Makri, S., Perrot, S., Sarzi-Puttini, P., Taylor, A., & Jones, G. T. (2017). EULAR revised recommendations for the management of fibromyalgia. Annals of the Rheumatic Diseases, 76(2), 318–328. https://doi.org/10.1136/annrheumdis-2016-209724