Motion is Lotion: Why Movement is Essential for Injury Recovery

For many years, injury recovery was synonymous with rest. Patients were often advised to stop activity altogether and allow the body to heal passively. However, current evidence and clinical practice have shifted toward a more active approach. The concept of “motion is lotion” reflects a growing understanding that appropriate, controlled movement plays a critical role in recovery, rather than prolonged inactivity.
Why Movement Matters in Healing
Movement supports the body’s natural healing processes in several important ways. When individuals move, circulation increases, delivering oxygen and nutrients to injured tissues while helping remove metabolic waste. This process can reduce stiffness, improve joint mobility, and accelerate tissue repair. Even low-intensity activity can help prevent lethargy and promote recovery, emphasizing that complete rest is rarely the optimal strategy (Chhabra, 2024). From a research standpoint, structured exercise programs have consistently demonstrated improvements in pain and function in patients with musculoskeletal conditions, particularly when they include a combination of strengthening, stretching, and aerobic components (Fransen et al., 2015; Bennell et al., 2017).
From R.I.C.E to PEACE & LOVE
Traditional injury management followed the R.I.C.E. principle: rest, ice, compression, and elevation. While still useful in certain situations, modern rehabilitation has evolved toward the PEACE & LOVE framework, which promotes a more balanced and active recovery strategy. PEACE focuses on early protection and education, while LOVE emphasizes the importance of gradual loading, optimism, vascularization, and exercise. This model encourages “relative rest,” meaning patients avoid aggravating activities but continue to engage in safe, modified movement. Evidence supports this approach, showing that progressive loading and exercise-based rehabilitation improve outcomes in both acute and chronic conditions, including osteoarthritis (Bennell et al., 2016; Messier et al., 2013).
What Does an Effective Exercise Program Look Like?
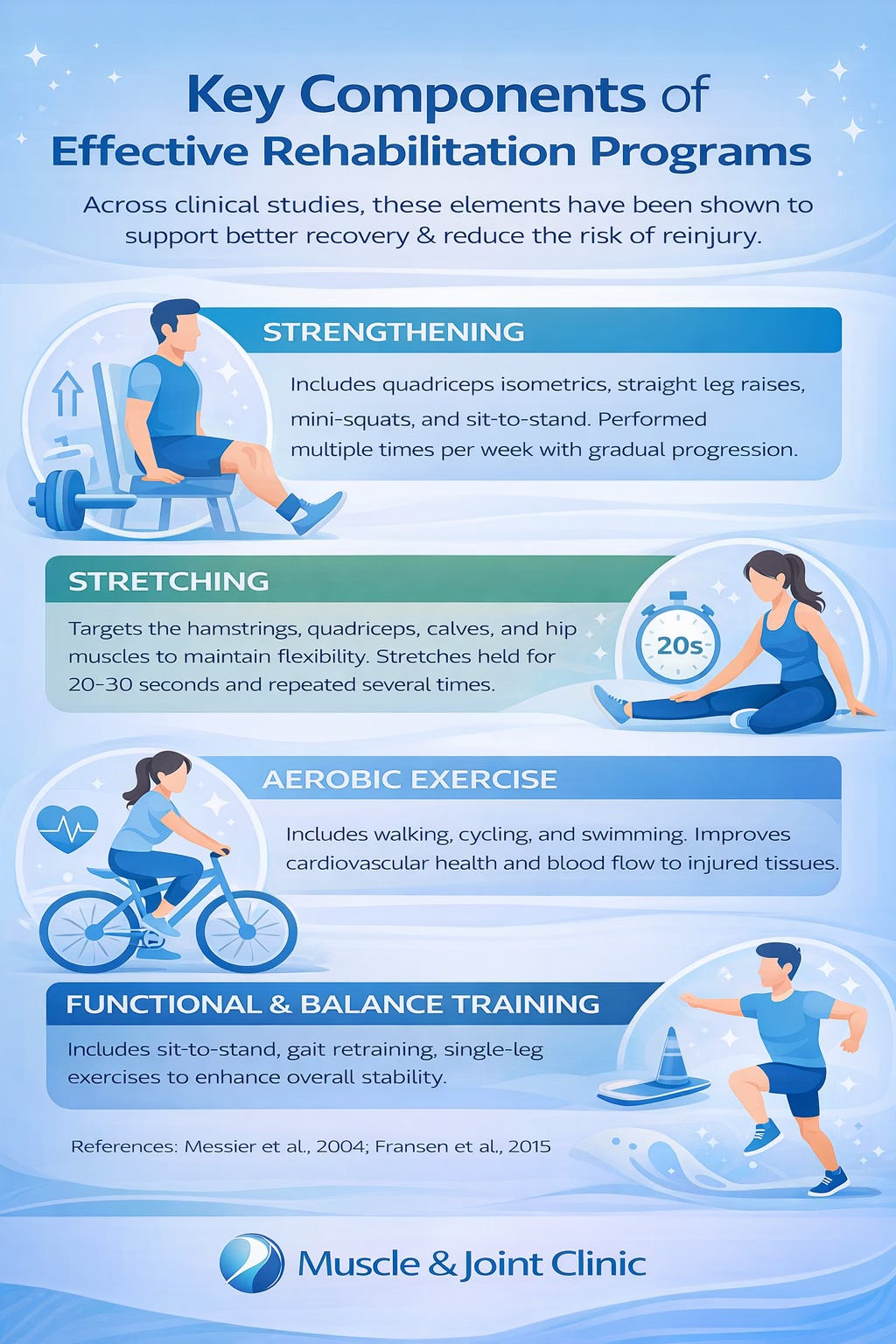
Across a wide range of clinical studies, effective rehabilitation programs share several common components. Strengthening exercises are the foundation, with a strong emphasis on the quadriceps and surrounding stabilizing muscles. Exercises such as quadriceps isometrics, straight leg raises, mini-squats, and sit-to-stand movements are frequently prescribed. These are typically performed multiple times per week with gradual progression in resistance, helping to reduce joint load and improve overall stability. Stretching is also an essential component, targeting the hamstrings, quadriceps, calves, and hip musculature to maintain flexibility and reduce stiffness. Most protocols recommend holding stretches for 20 to 30 seconds and repeating them several times per session.
In addition to strengthening and flexibility, aerobic exercise plays a key role in recovery. Low-impact activities such as walking, cycling, and swimming help improve cardiovascular health while enhancing blood flow to injured tissues. Research shows that combining aerobic exercise with strengthening leads to better long-term outcomes compared to isolated interventions (Messier et al., 2004; Fransen et al., 2015). Many programs also incorporate functional and balance training, including sit-to-stand movements, gait retraining, and single-leg stability exercises. These components help patients return to daily activities safely and reduce the risk of reinjury.
The Role of Home Exercise Programs (HEP)
Consistency is one of the most important factors in successful rehabilitation. Many studies emphasize the effectiveness of home exercise programs when patients are properly educated and supported. These programs often include a combination of strengthening, stretching, and mobility exercises performed at least three times per week, and in some cases daily. The use of visual guides, such as exercise cards or handouts, has been shown to improve adherence and ensure proper technique. Patients who consistently follow home exercise programs demonstrate meaningful improvements in both pain and function, even when supervision is limited (Cheawthamai et al., 2014; Kholvadia et al., 2019).
Mindset and Recovery
Recovery is not solely a physical process; psychological factors play an equally important role. Patients who understand their condition and actively participate in their rehabilitation tend to achieve better outcomes. Having a clear plan and structured approach provides reassurance and helps individuals feel empowered rather than limited by their injury. This active participation can improve motivation, adherence, and overall recovery experience (Chhabra, 2024).
When to Be Cautious
While movement is beneficial, it must be applied appropriately. Certain injuries, such as fractures, severe acute trauma, or neurological conditions, require careful evaluation before initiating activity. Pain should be used as a guide during rehabilitation. Mild discomfort may be acceptable, but sharp or worsening pain should be avoided. A tailored plan developed by a healthcare professional ensures that movement supports healing without increasing the risk of further injury.
Final Thoughts: Movement as Medicine
The evidence is clear that rest alone is no longer the gold standard for recovery. Instead, strategic and progressive movement is one of the most effective tools for restoring function and reducing pain. Exercise-based rehabilitation improves circulation, strengthens supporting structures, and enhances overall physical capacity. Whether recovering from an acute injury or managing a chronic condition, incorporating movement in a controlled and structured manner can significantly improve outcomes and help individuals return to their daily activities with confidence.
References (APA Style)
Bennell, K. L., Egerton, T., Pua, Y. H., Abbott, J. H., Sims, K., Metcalf, B., … & Hunter, D. J. (2016). Effect of physical therapy on pain and function in knee osteoarthritis. JAMA, 315(19), 1987–1997.
Bennell, K. L., Nelligan, R., Dobson, F., Rini, C., Keefe, F., Kasza, J., … & Hinman, R. S. (2017). Effectiveness of an internet-delivered exercise and pain-coping skills training intervention for persons with chronic knee pain. Annals of Internal Medicine, 166(7), 453–462.
Chhabra, S. (2024, April 27). “Motion is lotion”: Experts encourage movement to aid injury recovery. CBC Radio. https://www.cbc.ca
Cheawthamai, C., et al. (2014). Effects of home-based exercise programs in knee osteoarthritis patients.
Fransen, M., McConnell, S., Hernandez-Molina, G., & Reichenbach, S. (2015). Exercise for osteoarthritis of the knee. Cochrane Database of Systematic Reviews, (1).
Kholvadia, M., et al. (2019). Rehabilitation-based exercise protocols for knee osteoarthritis.
Messier, S. P., et al. (2004). Exercise and dietary weight loss in overweight and obese older adults with knee osteoarthritis. Arthritis & Rheumatism, 50(5), 1501–1510.
Messier, S. P., Mihalko, S. L., Legault, C., et al. (2013). Effects of intensive diet and exercise on knee joint loads, inflammation, and clinical outcomes among overweight and obese adults with knee osteoarthritis. JAMA, 310(12), 1263–1273.