Why the Front of the Knee Becomes Swollen, Warm, and Painful
Understanding Prepatellar Bursitis
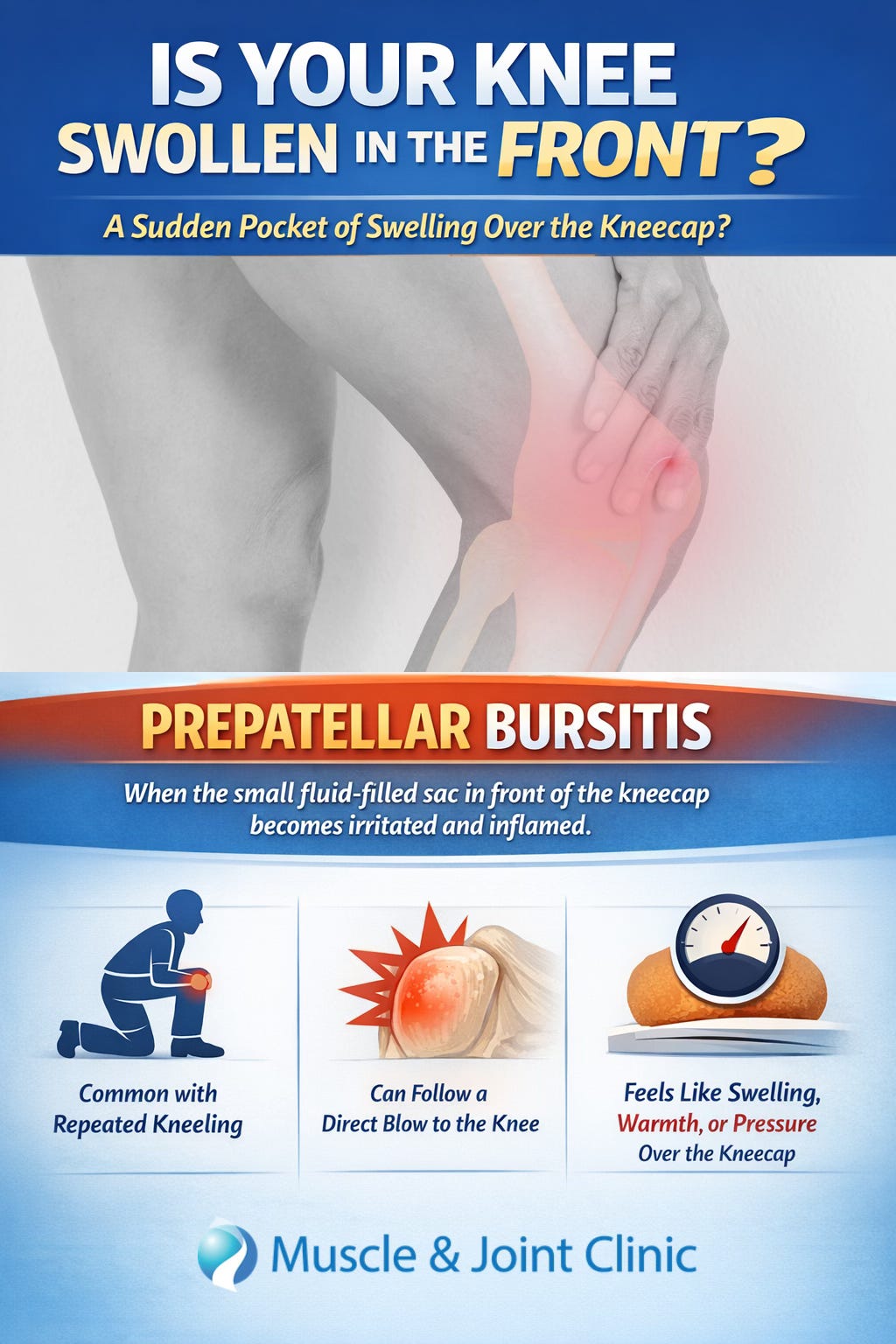
If you have ever noticed a sudden pocket of swelling at the front of your knee, especially right over the kneecap, one possible cause is prepatellar bursitis. This condition happens when the small fluid-filled sac in front of the kneecap, called the prepatellar bursa, becomes irritated and inflamed. The bursa normally helps reduce friction between the skin and the kneecap, but when it is aggravated, it can fill with extra fluid and become swollen, warm, and uncomfortable. In some cases, the area may feel more like pressure or tightness than sharp pain.
Prepatellar bursitis is often linked to repeated kneeling or pressure on the front of the knee, which is why it has sometimes been called “housemaid’s knee.” It can also happen after a direct blow to the knee, a sudden flare of inflammation, or sometimes without a clear cause that the patient can identify. In certain cases, it may also be related to inflammatory conditions such as gout or rheumatoid arthritis. Less commonly, the bursa can become infected, which is more serious and needs prompt medical attention (Aaron et al., 2011; Khodaee, 2017).
Many people with prepatellar bursitis notice swelling at the front of the knee that seems to come on quickly. The area may look puffy, feel warm to the touch, and become more uncomfortable when kneeling, bending the knee deeply, or putting pressure on it. Some cases are mild and annoying, while others can make walking, working, exercising, or even basic daily activities more difficult. One important point is that not every swollen knee is the same. Sometimes swelling over the kneecap is simply an irritated bursa, but in other cases it can overlap with cellulitis, joint inflammation, crystal-related flare-ups, or infection, which is why an accurate assessment matters (Baumbach et al., 2014; Khodaee, 2017).
A big part of evaluating prepatellar bursitis is determining whether it is septic or non-septic. Non-septic bursitis means the bursa is inflamed but not infected. Septic bursitis means infection is present, and that changes treatment significantly. Signs that may raise concern for infection include significant warmth, redness, skin damage over the area, fever, worsening pain, or feeling generally unwell. Infection is more likely in people with certain health conditions such as diabetes, kidney disease, or reduced immune function, but it can also happen in otherwise healthy individuals, especially after skin irritation or trauma near the knee (Brown et al., 2022; Khodaee, 2017).
Diagnosis usually starts with a careful history and physical examination. Sometimes the clinical picture is fairly clear, but imaging such as ultrasound can be very helpful when there is a lot of swelling or when the provider wants to confirm that the bursa is the source of the problem. Ultrasound can also help distinguish bursitis from surrounding soft tissue conditions like cellulitis and can guide aspiration if needed. If infection is suspected, the bursa may need to be aspirated so the fluid can be tested for white blood cells, bacteria, glucose, and crystals. Blood tests may also be used to support the assessment, especially when infection or a systemic inflammatory condition is part of the differential diagnosis (Baumbach et al., 2014; Khodaee, 2017).
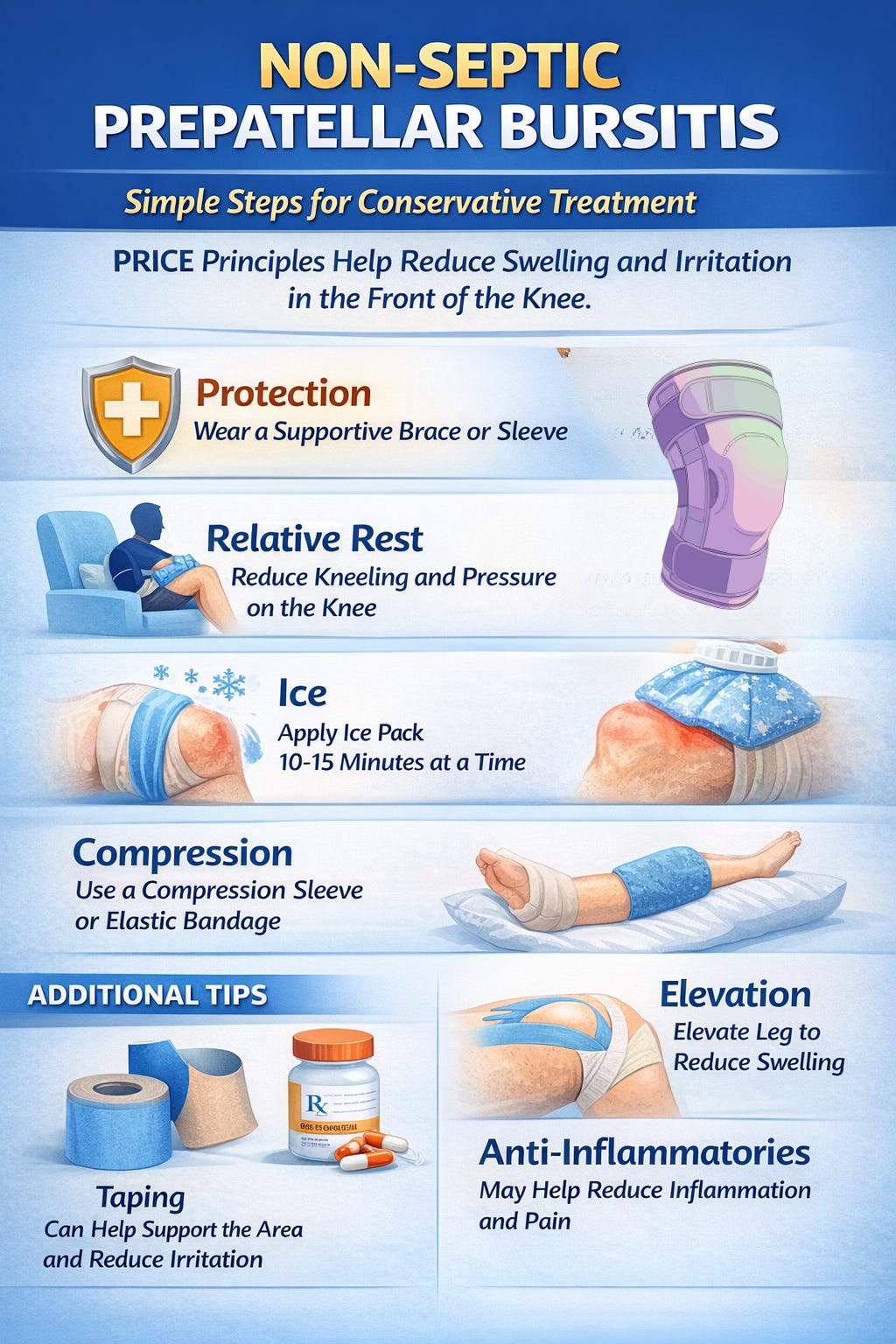
For non-septic prepatellar bursitis, conservative treatment is usually the best place to start. This often includes PRICE principles: protection, relative rest, ice, compression, and elevation. Reducing kneeling and avoiding repeated pressure on the front of the knee can make a big difference. Bracing or a compression sleeve may help control swelling and improve comfort with walking and daily activities. Taping can also be useful in some cases as a way to support the area and reduce local irritation. Anti-inflammatory medication may be considered when appropriate, depending on the patient’s health history and medical guidance (Aaron et al., 2011; Khodaee, 2017).
At our clinic, conservative care for non-septic prepatellar bursitis may include chiropractic or physiotherapy-based support depending on the person’s presentation. In the early stages, the main goal is usually to calm the irritated tissues and avoid aggravating the bursa further. That may involve education, activity modification, supportive bracing, taping, and symptom-relieving modalities as short-term tools. As symptoms improve, care can shift toward addressing the mechanical factors that may have contributed to the problem in the first place. This might include improving lower extremity movement patterns, reducing excessive strain through the knee, and working on strength, mobility, and function so the person can return to regular activities more confidently. Passive modalities can sometimes help in the short term, but they work best when paired with a more active recovery plan rather than being used on their own (Brown et al., 2022; Khodaee, 2017).
Not every case needs aspiration or injection. In fact, aspiration is generally not recommended for clearly non-infectious chronic microtraumatic bursitis because there is a risk of introducing infection into the bursa. Corticosteroid injections have been used in some cases, but the research supporting routine use is limited, and there are risks to consider. More persistent or recurrent cases may need additional medical evaluation, and in select situations surgical treatment is considered, especially when swelling keeps coming back or significantly interferes with function (Aaron et al., 2011; Baumbach et al., 2014; Khodaee, 2017).
When the bursitis is septic, treatment is different. These cases usually require aspiration and antibiotics, and more severe cases may need hospital-based care or surgical drainage. Because infection can sometimes worsen quickly, persistent warmth, redness, spreading swelling, severe tenderness, or fever should not be ignored. This is especially important when the knee becomes increasingly painful or the person starts to feel systemically unwell (Brown et al., 2022; Khodaee, 2017).
The main takeaway is that prepatellar bursitis is often manageable, but it should not be dismissed as “just knee swelling.” The front of the knee can swell for different reasons, and the right treatment depends on the cause. For many non-septic cases, conservative care with PRICE, bracing, taping, activity modification, and a gradual return to movement works well. Chiropractic and physiotherapy care can help support recovery by reducing stress on the irritated tissues and improving how the knee is functioning overall. The key is making sure the condition is properly assessed first, especially when warmth, redness, or significant swelling are present.
References
Aaron, D. L., Patel, A., Kayiaros, S., & Calfee, R. (2011). Four common types of bursitis: Diagnosis and management. The Journal of the American Academy of Orthopaedic Surgeons, 19(6), 359–367. https://doi.org/10.5435/00124635-201106000-00006
Baumbach, S. F., Lobo, C. M., Badyine, I., Mutschler, W., & Kanz, K. G. (2014). Prepatellar and olecranon bursitis: Literature review and development of a treatment algorithm. Archives of Orthopaedic and Trauma Surgery, 134(3), 359–370. https://doi.org/10.1007/s00402-013-1882-7
Brown, O. S., Smith, T. O., Parsons, T., Benjamin, M., & Hing, C. B. (2022). Management of septic and aseptic prepatellar bursitis: A systematic review. Archives of Orthopaedic and Trauma Surgery, 142(10), 2445–2457. https://doi.org/10.1007/s00402-021-03853-9
Khodaee, M. (2017). Common superficial bursitis. American Family Physician, 95(4), 224–231.